KAREO BILLING Insurance Enrollments
Submit claims, check eligibility, and receive ERAs electronically.
 Insurance Enrollments
view details
Insurance Enrollments
view details view less
view less
Insurance Enrollments can be cumbersome and time consuming, with a mess of complex paper trails. Kareo Insurance Enrollments lessens the burden of antiquated enrollment processes. Once you complete your Electronic Data Interchange (EDI) enrollment, Kareo Billing makes it easy for billers and system administrators to submit claims and other transactions effortlessly, creating a smooth, traceable system that works closely with our clearinghouse partners. In fact, Kareo enables connections for over 8,000 insurance companies. The TAF (Transfer of Authorization) form enables Kareo to act on behalf of Providers to assist in completing successful enrollments. With the average American practice managing up to 25-40 payers at a time, this saves time, so you can focus on delivering the best quality of care.
Checking eligibility, submitting claims and receiving ERAs digitally drastically reduces the amount of time you spend on these tasks. It enables your practice to see in real-time the status of your insurance enrollments, allowing for transparency throughout the process. And you have a dedicated team of specialists available at Kareo to help guide you. Electronic submissions are also eco-friendly!
Kareo offers three different electronic services, including:
- Claims Submission: Say goodbye to antiquated, time-consuming paper-based patient claims that get lost in the mail. Kareo allows for an instant electronic submission direct to the clearinghouse and on to the payer, and allows for modifications in-process, if needed.
- Eligibility Checks: Use Kareo to electronically verify your patient’s eligibility before you render your services. By submitting quicker claims, your practice can receive faster reimbursement.
- Electronic Remittance Advice (ERA): Once enrolled in ERAs, you can receive medical insurance payment explanations electronically. This saves time compared to manual mail processes.
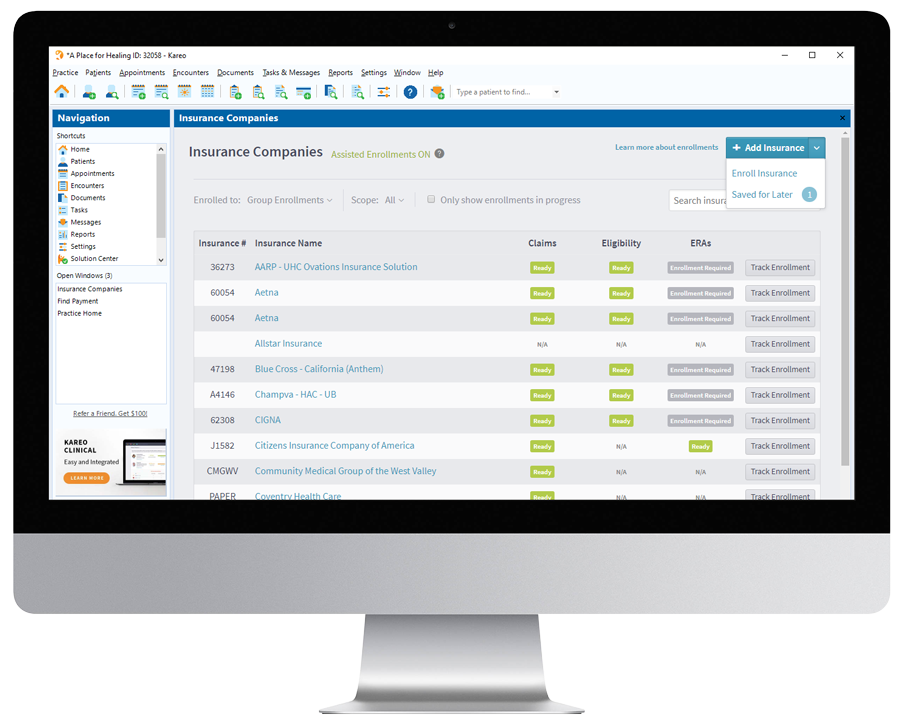
Kareo Billing includes highly-visual statuses of enrollment.
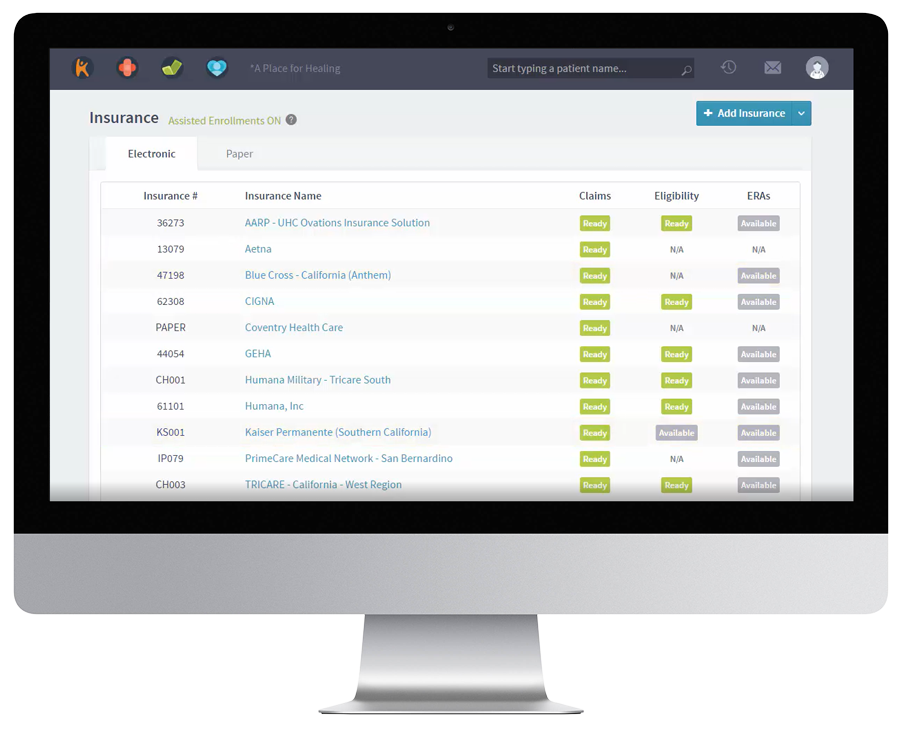
Administrators within Kareo Clinical also have insight into the status of enrollments.
Billing Efficiency from the Start
Quickly and easily add insurance from Kareo’s commonly requested insurance list, or use the streamlined search functionality to find insurances. Plus, it's easy to add custom insurance companies.
Simple Set-up for Billers and Practices
Kareo’s electronic enrollment set-up is a simple, 6 step process that guides you every step of the way.
Faster Enrollments & Reimbursements with Less Effort
With digital processes, your team spends less time putting together paper forms and waiting for snail mail returns. Plus, they'll gain peace of mind with email confirmations and visual status updates directly from the Electronic Enrollments Dashboard.
For peace of mind, Kareo provides a transparent tracking view of specific insurance enrollments.
FEATURES
With Kareo, enrollments are a simple and intuitive experience:
- Electronic Claims Submission – Leave paper forms and snail-mail behind. You'll free up time, save precious desk space , and improve accuracy. Kareo also supports electronic submission of workers compensation claims that include up to 10 pages of documentation saving you time and money.
- Electronic Eligibility Checks – With electronic eligibility checks, your front office doesn't need to sit on the phone waiting to approve eligibility. They can do it in advance, before patients arrive in the office.
- Electronic Remittance Advice (ERAs)- Kareo saves you hours of data entry with electronic posting. You can even post numerous insurance payments at once.
- Transfer of Authorization Form (TAF)- Kareo has connections with over 8,000 insurance companies through our clearinghouse partners, relieving you of the burden of managing dozens of payers. Let Kareo facilitate your enrollments with a simple TAF.
- Tracking – The Kareo Dashboard gives you 100% transparency with step-by-step visual confirmations of enrollment statuses from request to submission to completion. See pertinent information, like case numbers, estimated dates for payer response and activity history.




