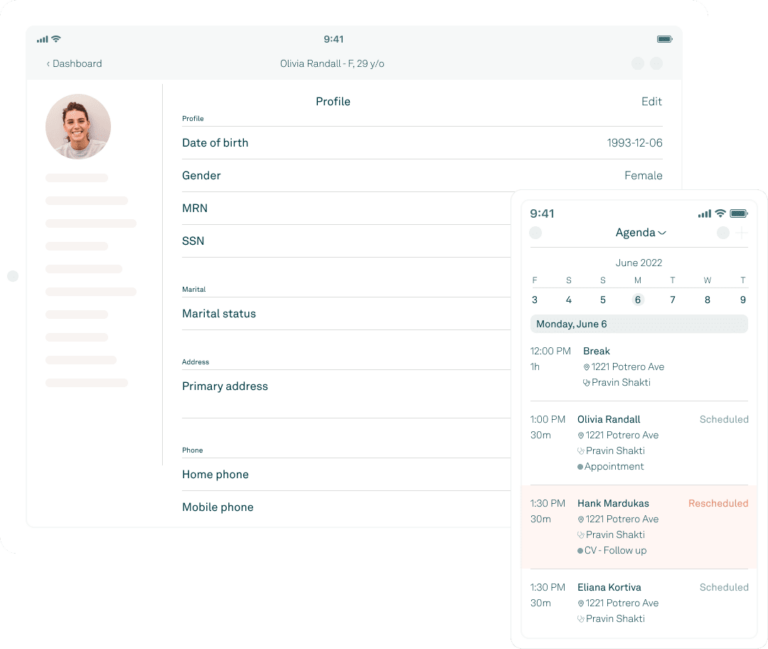
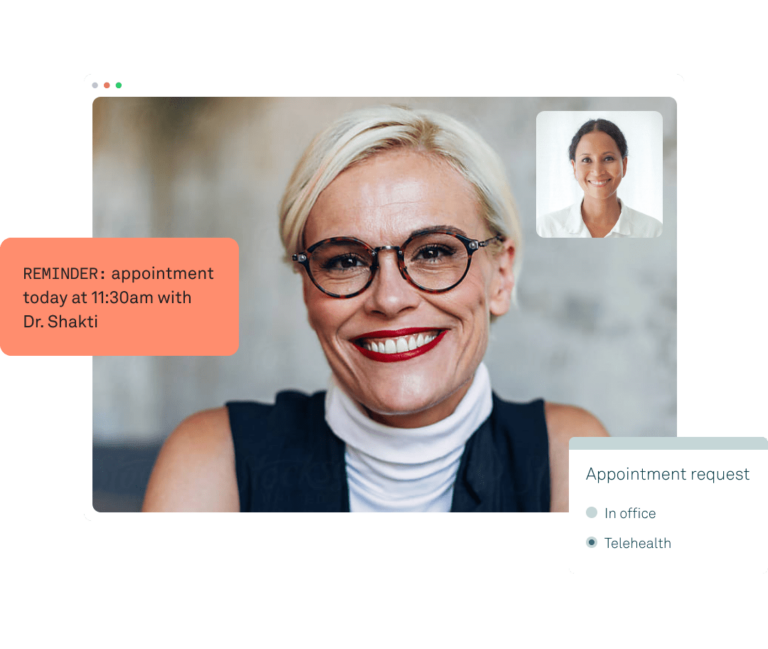
Electronic health records
Support your practice’s entire clinical workflow and control how you deliver care with Tebra’s cloud-based, ONC-certified electronic health record (EHR).
Frequently asked questions
-
Why should I choose Tebra’s EHR over another EHR?
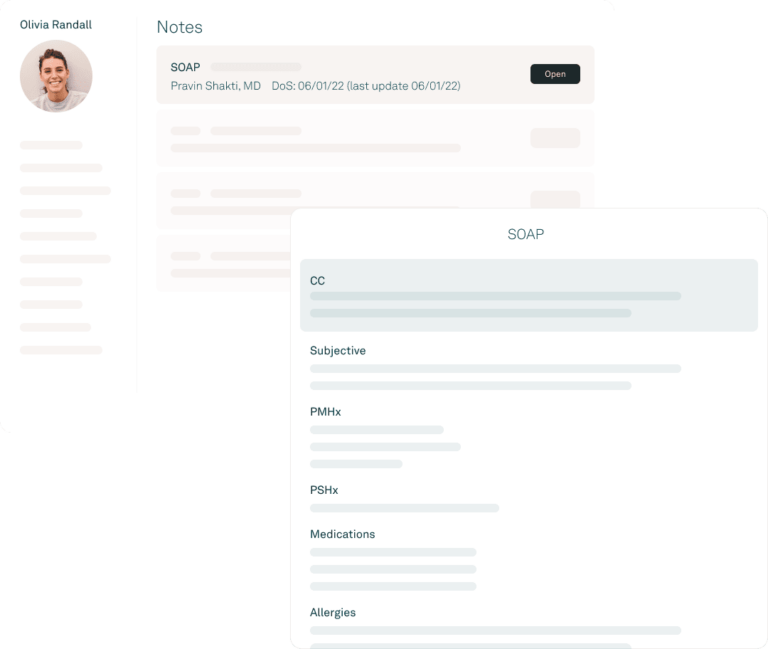
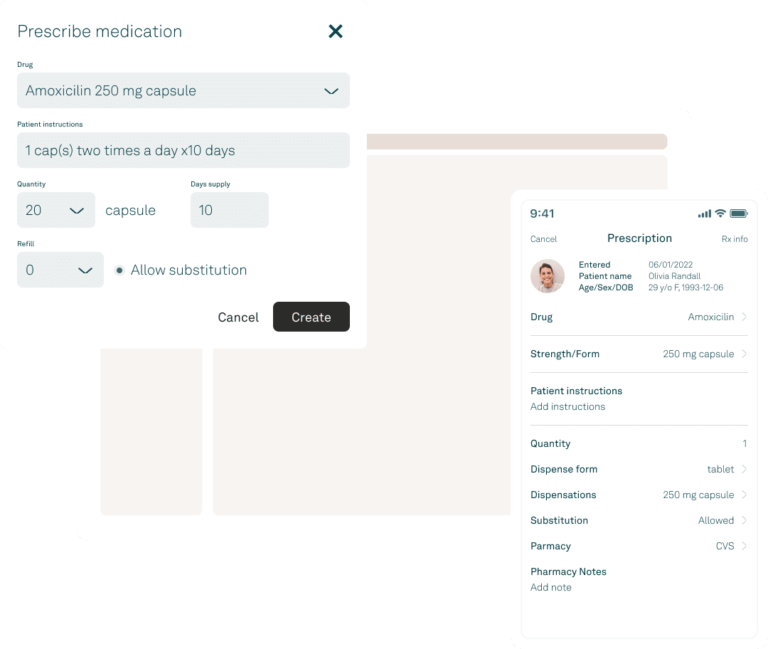
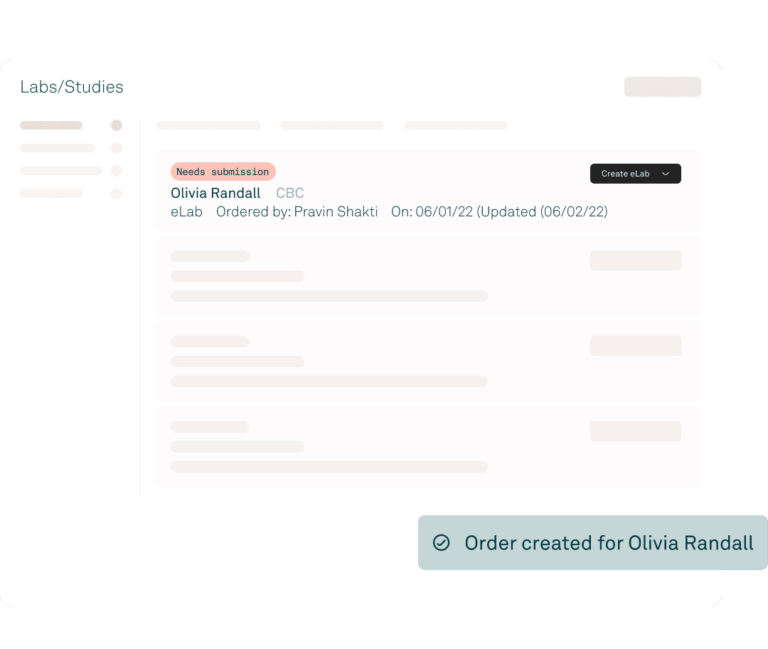
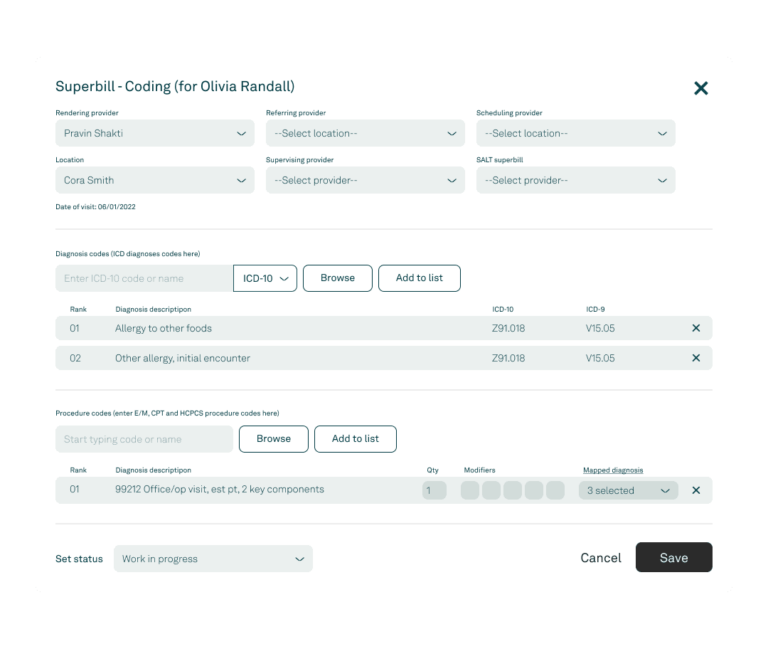
Tebra’s EHR is built just for independent practices and was designed by healthcare providers, so it has the key features you want and is surprisingly easy to use. Write a note, prescribe a medication, view electronic medical records, and create a superbill in just minutes. Plus, we offer full customer service and training support free of charge.
-
How does the integration between Clinical and Billing work?
We write patient records, insurance information, and appointments to the same database so you’re always in sync. We seamlessly push superbills from Clinical to Billing and automatically scrub your claims to improve the success of your billing process. According to MGMA, using integrated technology like Tebra can improve your overall revenue by nearly 10%.
-
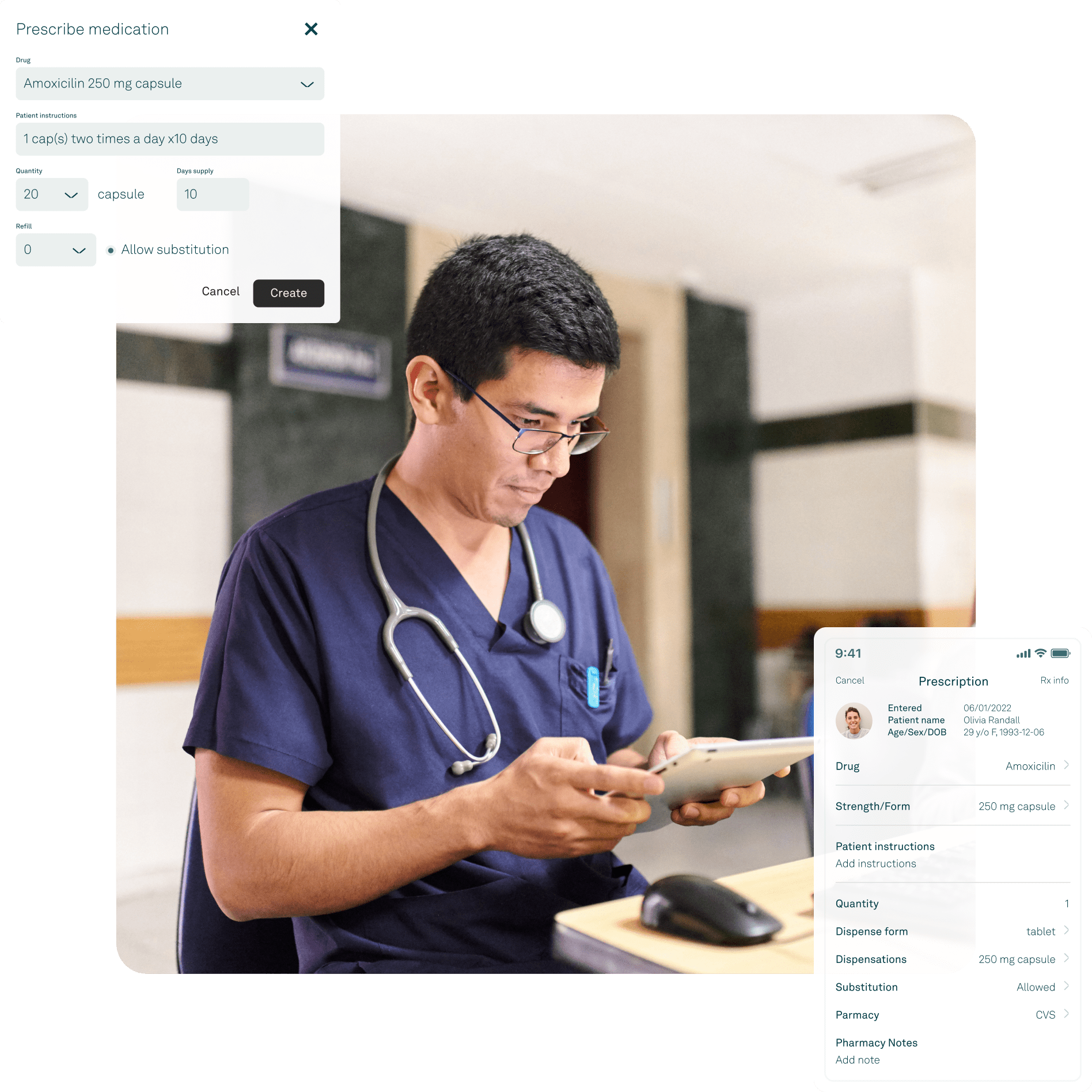
Will my local pharmacy be listed in the EHR?
We electronically prescribe to over 50,000 pharmacies across the United States by partnering with SureScripts. As a very small number of local pharmacies don’t yet accept electronic prescriptions, you can still print prescriptions for patients if their pharmacy is not listed.
-
Are there specific system requirements to use Tebra’s EHR?
Our EHR is cloud-based, so all you need is a computer (PC or Mac, laptop or desktop) with an up-to-date web browser (we recommend Firefox or Google Chrome) and a high-speed internet connection.
-
Is Tebra’s EHR certified for meaningful use?
Yes! It is 2014 Edition certified by the Drummond Group for both Stage 1 and Stage 2. Kareo’s CMS EHR Certification ID is: A014E01NDGFDEAD.